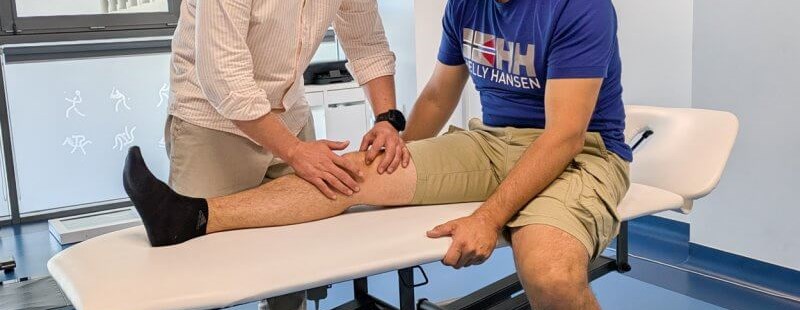
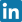What is Lateral Patellar Compression Syndrome?
Lateral patellar compression syndrome (ELPS) is a biomechanical disorder in which the lateral aspect of the patellofemoral joint is chronically overloaded. Due to improper alignment or tracking of the patella within the femoral trochlear groove, pressure increases on the lateral facet of the patella, potentially resulting in cartilage damage and degenerative changes. ELPS is not a distinct disease entity but rather a symptom complex stemming from muscular imbalance and anatomical predisposition.
It most commonly affects young individuals but may also occur in older adults due to degenerative changes. The syndrome is often mistaken for other causes of anterior knee pain, complicating proper diagnosis. Imaging studies and a thorough biomechanical evaluation are essential for accurate diagnosis. If left untreated, ELPS can lead to progressive damage to the peripatellar structures and worsening of knee joint function. Understanding the nature of this condition is key to implementing effective conservative or surgical treatment.
Causes of Lateral Patellar Compression
- Muscle imbalance – Weakness of the vastus medialis obliquus (VMO) combined with tightness of the vastus lateralis causes the patella to be pulled laterally.
- Tight lateral structures – Shortening of the lateral retinaculum or the iliotibial band can cause persistent lateral displacement of the patella, restricting its proper tracking.
- Anatomical abnormalities – A shallow femoral trochlear groove (trochlear dysplasia) or high-riding patella (patella alta) increases the risk of developing the condition.
- Knee valgus – Excessive inward angulation of the knees alters the mechanical axis of the lower limb, increasing lateral patellar pressure.
- Previous injuries or overuse – Recurrent microtrauma or prior knee injuries may lead to lasting changes in soft tissue tension and patellar tracking.
- Incorrect movement patterns – Faulty technique in running, jumping, or resistance training can overload the patellofemoral joint and contribute to secondary dysfunction.
Symptoms of Lateral Patellar Compression Syndrome
- Anterior knee pain (patellofemoral pain) – The most common symptom is pain in the front of the knee, worsening during activities that load the patellofemoral joint, such as stair climbing, squatting, or rising from a seated position.
- Pain during prolonged sitting with bent knees – Discomfort after prolonged sitting with flexed knees, typical during long trips or movie watching.
- Sensation of "grinding" or "popping" of the patella – Patients may experience abnormal patellar movement, rubbing, clicking, or popping during knee flexion and extension.
- Increased tension on the lateral side of the knee – A feeling of tightness or pulling on the outer side of the patella, often due to lateral retinacular tightness.
- Weakness and a sense of knee instability – A sensation that the knee is weak, “giving way,” or lacking full control, especially during direction changes.
- Reduced range of motion – Difficulty fully flexing or extending the knee due to pain or mechanical blockage of the patella.
- Lack of swelling or minimal inflammation – Unlike acute injuries, ELPS typically does not cause significant swelling; the changes are more functional than inflammatory.
- Bilateral symptoms – Both knees are often affected, although symptoms may be more pronounced on one side.
Diagnosis of Lateral Patellar Compression Syndrome
Diagnosis of ELPS relies on a detailed clinical history, functional assessment, and imaging studies that together help identify patellar maltracking and misalignment. During physical examination, attention is focused on patellar tracking during flexion and extension, tension in the lateral retinaculum, and the strength and activation of the vastus medialis obliquus (VMO). The patellar tilt test may reveal tenderness and restricted medial patellar mobility, suggesting lateral soft tissue tightness. Evaluating lower limb biomechanics—such as pelvic alignment, knee axis, and foot positioning—is also essential, as abnormalities in these structures may contribute to patellofemoral dysfunction.
In imaging diagnostics, magnetic resonance imaging (MRI) plays a crucial role in assessing cartilage integrity, soft tissue structures, and identifying patellofemoral joint damage. Computed tomography (CT) allows for precise measurement of the lateral patellar tilt angle and evaluation of patellar rotation and femoral trochlear dysplasia. X-rays (in Merchant, Laurin, or skyline views) provide insight into patellar height and its position relative to the trochlear groove. A comprehensive diagnostic approach is necessary, as ELPS often coexists with other causes of anterior knee pain and may be difficult to distinguish without full anatomical and functional analysis.
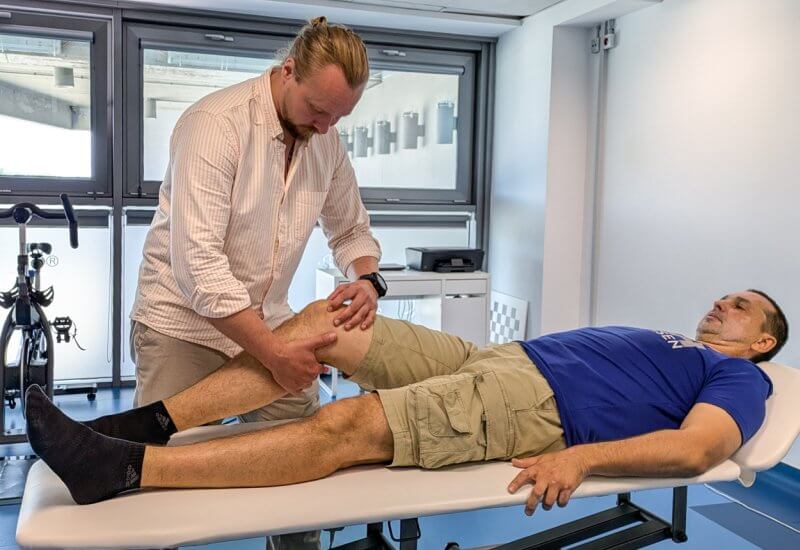
Conservative Treatment of Lateral Patellar Compression Syndrome
Conservative (non-surgical) treatment is the most commonly used and effective approach for mild to moderate cases of ELPS, particularly in patients without significant anatomical abnormalities. The cornerstone of therapy is individualized physical therapy aimed at restoring muscular balance—primarily strengthening the vastus medialis obliquus (VMO) and stretching tight lateral structures (lateral retinaculum, iliotibial band).
Additional supportive therapies include:
- Taping – To guide and improve patellar tracking.
- Orthotic inserts or foot biomechanics correction – In cases of faulty foot alignment (e.g., overpronation).
- Pharmacologic treatment – Nonsteroidal anti-inflammatory drugs (NSAIDs) during acute pain episodes.
- Temporary activity modification – Avoiding patellofemoral loading activities.
In some cases, intra-articular injections (e.g., hyaluronic acid, platelet-rich plasma – PRP) are used to improve cartilage quality and relieve pain. Conservative treatment typically lasts several weeks to months and results in significant functional improvement and pain reduction in most patients.
Surgical Treatment of Lateral Patellar Compression Syndrome
Surgical intervention is considered when conservative management fails to yield improvement after at least 3–6 months, or when there are significant anatomical abnormalities that cannot be addressed through rehabilitation alone. The main goals of surgery are to reduce tension in lateral structures, improve patellar alignment, and restore proper tracking.
Common surgical techniques include:
- Lateral release – Involves cutting tight lateral tissues to allow the patella to shift medially. This procedure is now performed selectively and often in combination with other interventions.
- Medial patellofemoral ligament (MPFL) reconstruction – Indicated for patients with patellar instability to enhance medial stabilization and prevent lateral maltracking.
- Tibial tubercle osteotomy (e.g., Fulkerson technique) – Used when significant mechanical axis deviations and tracking abnormalities are present. It involves repositioning the patellar tendon insertion to correct patellar trajectory.
- Trochleoplasty – Reserved for cases of trochlear dysplasia with a shallow groove, increasing patellar instability. This invasive procedure is indicated in patients with severe anatomical deformities.
Postoperative Rehabilitation
Rehabilitation following surgical treatment of ELPS is a complex process requiring close collaboration among the patient, physiotherapist, and orthopedic surgeon. The primary goals are to restore knee joint function, stabilize the patella, and prevent recurrence. The rehabilitation process depends on the type of surgery performed.
1. Early Phase (0–2 weeks post-op)
Focus on limb protection, pain and swelling control, and prevention of complications (e.g., thrombosis). The knee is usually immobilized in a brace allowing controlled flexion, and ambulation is performed with crutches under partial weight-bearing. Gentle quadriceps isometric exercises and limited range of motion are initiated.
2. Range of Motion Restoration Phase (2–6 weeks)
Gradually increase knee joint range of motion aiming for full extension and approximately 90–120° of flexion. Mobilization exercises, unloaded active movements, and gentle strengthening of the quadriceps, gluteals, and pelvic stabilizers are introduced. Weight-bearing is progressively increased depending on surgical specifics and healing status.
3. Muscle Strength and Neuromuscular Control Phase (6–12 weeks)
Focus on restoring muscle strength—particularly of the VMO—and improving motor control. Functional exercises such as unloaded squats, treadmill walking, stationary cycling, and proprioceptive/balance training are implemented. More complex movement patterns and increased loads are introduced based on individual progress.
4. Return to Activity Phase (from week 12 onward)
The final phase targets safe return to daily and sports-specific activities. It includes dynamic drills, plyometric training, running, and progressive reintroduction of sport-specific movements. Functional testing is used to assess knee strength, stability, and motor control prior to full return to activity. Return to sports typically occurs after 4–6 months, though in more complex cases it may take 9–12 months.