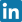What is spinal stenosis?
Spinal stenosis, also known as narrowing of the spinal canal, is a condition in which the space within the spine becomes constricted. This leads to pressure on the spinal cord and nerves, causing various symptoms such as back pain, limb numbness, or walking difficulties. The causes are diverse but primarily include degenerative changes, including intervertebral disc degeneration.
Stenosis may affect various regions of the spine, most commonly the:
- Lumbar spine – leading to lower back pain, leg weakness, and symptoms that worsen during walking (known as neurogenic claudication).
- Cervical spine – may cause cervical myelopathy, leading to neurological disturbances in both upper and lower limbs.
- Thoracic spine – can significantly impair motor function.
Regardless of the origin, spinal stenosis can greatly impact quality of life, which is why it is important to seek specialized care, such as the services offered at Rehasport.
Causes of Spinal Stenosis
Degenerative changes in the spine Degeneration is the most common cause, especially in individuals over 50. Factors contributing to spinal canal narrowing include:
a) Hypertrophied ligaments
The ligamentum flavum can thicken in response to chronic mechanical stress, reducing the space for the spinal cord and nerve roots.
b) Facet joint degeneration and hypertrophy
The facet joints may degenerate due to cartilage wear and inflammation, leading to osteophyte formation that can compress neural structures.
c) Degeneration of intervertebral discs
Intervertebral discs lose hydration and height with age, causing segmental instability, disc bulging into the spinal canal, and secondary canal narrowing.
d) Degenerative spondylolisthesis
This involves the slippage of one vertebra over another due to weakened stabilizing structures, causing spinal canal narrowing and nerve compression.
Congenital predisposition to a narrow spinal canal
Some individuals are born with a narrower spinal canal. While not always symptomatic, this can predispose them to stenosis, particularly when combined with other risk factors.
Inflammatory spinal diseases
a) Rheumatoid arthritis (RA) – an autoimmune disease that attacks joints, including spinal joints, leading to inflammation, cartilage destruction, and scarring that narrows the canal.
b) Ankylosing spondylitis (AS) – involves progressive stiffening of the spine due to ligament and joint ossification, contributing to stenosis.
c) Gout and other metabolic diseases – crystal deposits, such as uric acid crystals, can cause joint hypertrophy and secondary stenosis.
Trauma and post-traumatic changes
a) Vertebral fractures – especially compression fractures in osteoporosis, may deform the spinal canal.
b) Scarring and adhesions post-injury or surgery – healing processes can result in fibrotic tissue that occupies spinal canal space.
c) Herniated intervertebral discs – can protrude into the canal, compressing the spinal cord or nerve roots.
Spinal infections and abscesses
Infections such as spinal tuberculosis (Pott's disease) or epidural abscesses can cause tissue swelling or instability, leading to canal narrowing.
Symptoms of Spinal Stenosis
1. Lumbar spinal stenosis:
a) Neurogenic claudication – pain, weakness, tingling, or heaviness in the legs while walking or standing, relieved by bending forward or sitting.
b) Low back pain – may be chronic or intermittent, often radiating to the buttocks, thighs, or calves; symptoms may be unilateral or bilateral and worsen with spine extension or prolonged standing.
c) Sensory disturbances and muscle weakness – including tingling, numbness, or "electric shock" sensations in the legs; in advanced cases, foot drop and muscle atrophy can occur.
d) Balance and coordination issues – in severe cases, patients may have difficulty walking on uneven surfaces.
2. Cervical spinal stenosis:
a) Neck pain radiating to shoulders and arms – often chronic or intermittent, worse with neck extension; may include stiffness.
b) Tingling and numbness in the arms – often affecting hands and fingers, impairing fine motor skills.
c) Muscle weakness and difficulty gripping objects – affecting both upper and lower limbs.
d) Gait and balance disturbances – coordination difficulties leading to unsteady, slow, or stumbling gait.
e) Cervical myelopathy – a severe complication potentially leading to permanent disability, including lower limb weakness, impaired mobility, and incontinence.
3. Thoracic spinal stenosis:
a) Mid-back pain – may radiate to the ribs and abdomen, worsens with trunk movement.
b) Sensory disturbances in the torso and legs – including tingling or numbness in the chest or abdomen, sometimes mimicking cardiac or gastrointestinal issues.
c) Leg weakness and walking difficulties – progressive lower limb weakness may cause gait disturbances.
When Should You See a Specialist?
Consult a specialist if you experience any of the following:
- Persistent lower back or neck pain, worsened by walking or standing.
- Neurogenic claudication (leg pain during walking that subsides with rest).
- Numbness, tingling, or weakness in the limbs.
- Balance issues or trouble walking.
- Reduced spinal mobility or stiffness.
Early intervention increases the chance of full recovery. Don’t wait until the symptoms become disabling—consult one of our experts today.
Diagnosis of Spinal Stenosis
Diagnosis begins with a thorough medical history, where an orthopedic specialist will ask about the pain’s nature, location, triggers, and associated symptoms like gait disturbances. A physical exam follows, assessing muscle strength, neurological reflexes, and spinal mobility. Testing for neurogenic claudication is a key indicator of lumbar stenosis.
Imaging tests include:
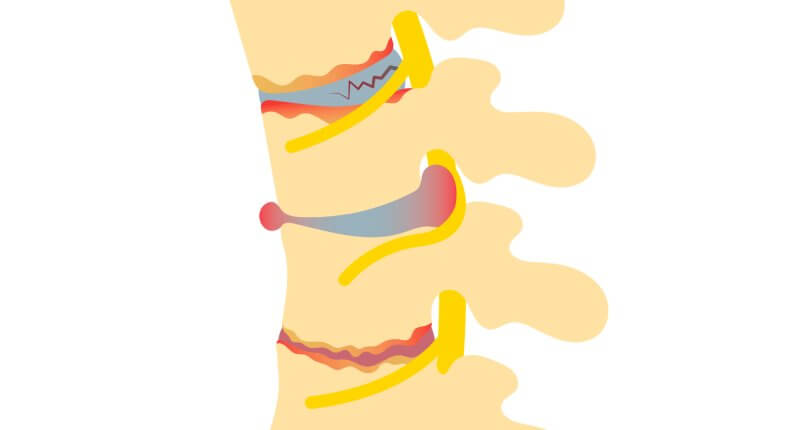
- Magnetic resonance imaging (MRI) – provides detailed views of the spinal canal, nerve compression, discs, and ligaments.
- Computed tomography (CT) – used when MRI is contraindicated (e.g., metal implants), often combined with myelography to visualize cerebrospinal fluid flow and canal narrowing.
- X-rays – less detailed but useful for spotting degenerative changes and spinal instability.
- Electromyography (EMG) – assesses nerve conduction to differentiate stenosis from other neurological disorders.
Non-Surgical Treatment
The first-line treatment focuses on symptom relief and quality of life improvement:
- Medications – including NSAIDs, pain relievers, and, in some cases, muscle relaxants or antidepressants for neuropathic pain.
- Physical therapy – aims to strengthen paraspinal muscles, improve flexibility, and offload the spine through targeted exercises.
- Epidural steroid injections – temporarily reduce inflammation and alleviate pain.
- Lifestyle changes – such as weight management, avoiding prolonged standing, and using proper movement techniques.
Conservative therapy is effective for many patients. However, in advanced stenosis or refractory cases, surgical intervention may be necessary.
Surgical Treatment
Surgery is considered when symptoms severely impair daily function and non-surgical methods fail. The goal is to relieve pressure on the spinal cord and nerves.
Common procedures:
- Decompressive laminectomy – removal of part of the vertebral arch to enlarge the spinal canal.
- Spinal fusion or instrumentation – to stabilize the spine when instability is present.
Minimally invasive techniques, such as endoscopic decompression, reduce implant use and promote quicker recovery.
Postoperative rehabilitation is essential for muscle strengthening, posture correction, and gradual return to activity. While surgery often improves pain and mobility, it carries inherent risks, and decisions are made based on disease severity and patient health.
Treatment Options at Rehasport
We offer individually tailored treatments, from non-invasive therapies (rehabilitation, physical therapy, medications) to surgical interventions when necessary. Treatment selection is based on disease severity and the patient's overall condition.
Risks and Complications of Spinal Surgery
Though generally safe and precise, spinal surgeries carry some risks. At Rehasport, we use advanced surgical techniques to minimize complications, with continuous care from experienced specialists to ensure the highest safety standards.
Is Rehabilitation Necessary After Treatment?
Yes, rehabilitation is crucial for full recovery. At Rehasport, we design personalized rehabilitation plans to strengthen muscles, improve mobility, and reduce recurrence risks.
Take Care of Your Health Today
Spinal stenosis can severely impact your quality of life, but early recognition and action can prevent worsening. The sooner you seek help, the better your chances of full recovery. At Rehasport, we offer comprehensive care and safe treatment methods to help you regain comfort and functionality. Don’t let pain limit your life—take action now.