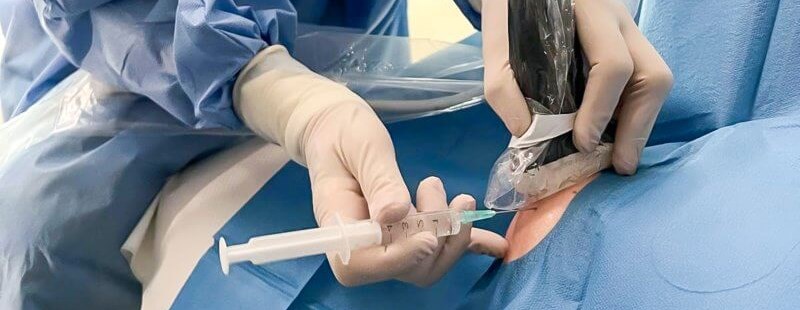
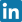What is Sonosurgery?
Sonosurgery, also known as interventional ultrasonography, involves performing precise, minimally invasive medical interventions under ultrasound guidance. This technique allows the physician to accurately locate pathological structures such as inflamed bursae, cysts, calcifications, or degenerated tendons, and perform targeted treatment without the need for conventional surgery.
The benefits of this approach include not only its low invasiveness but also rapid—and often immediate—restoration of function. Most procedures do not require hospitalization, and the patient can usually leave the clinic shortly after the intervention. Studies show that sonosurgery reduces the risk of complications and side effects, particularly when compared to traditional surgical methods. Importantly, this technique is being increasingly used not only in orthopedics but also in rheumatology and sports medicine, addressing the growing demand for effective yet safe therapeutic options.
What Procedures Can Be Performed Using Sonosurgery?
Aspiration and Drainage Under Ultrasound Guidance
These procedures allow for the safe and accurate removal of excess fluid from intra-articular or periarticular spaces (e.g., cysts, bursitis). Ultrasound guidance ensures precise needle placement, minimizing the risk of injury to adjacent structures.
Intra-Articular and Periarticular Injections
This involves the injection of medications (e.g., corticosteroids, hyaluronic acid, PRP – platelet-rich plasma, collagen) into pathologically altered tissues. Sonosurgery allows for precise drug delivery directly to the site of pathology, increasing treatment efficacy and reducing adverse effects.
Removal of Calcifications from Muscles and Tendons (Barbotage)
This technique is especially relevant for calcific tendinopathy in the rotator cuff. Under ultrasound guidance, the calcific deposits are fragmented, flushed, and aspirated, which significantly reduces pain and restores shoulder mobility. When combined with proper rehabilitation, it yields excellent outcomes.
Treatment of Ganglion Cysts
Instead of classic surgical excision, the cyst can be punctured and aspirated under ultrasound guidance. This can be combined with targeted administration of anti-inflammatory drugs, reducing the risk of recurrence.
Tenotomy – Tendon Release
In chronic overload or inflammatory conditions, especially involving the long head of the biceps tendon, a micro-incision or complete tenotomy can be performed using a needle under ultrasound control. This procedure reduces pain, particularly in older patients for whom surgical intervention carries higher risk.
Biologic Therapies – PRP, Stem Cells
Administering autologous preparations requires precise application to the site of injury (e.g., meniscal tear, tendon strain), which is ensured by ultrasound imaging.
Neuromodulation and Nerve Blocks
Precise injections targeting peripheral nerves (e.g., radial or suprascapular nerve) enable the treatment of chronic pain syndromes. Both diagnostic and therapeutic nerve blocks are used in this context.
Sonosurgery is rapidly evolving and represents a genuine alternative to many traditional surgical procedures—offering patients greater safety, shorter recovery time, and improved comfort.
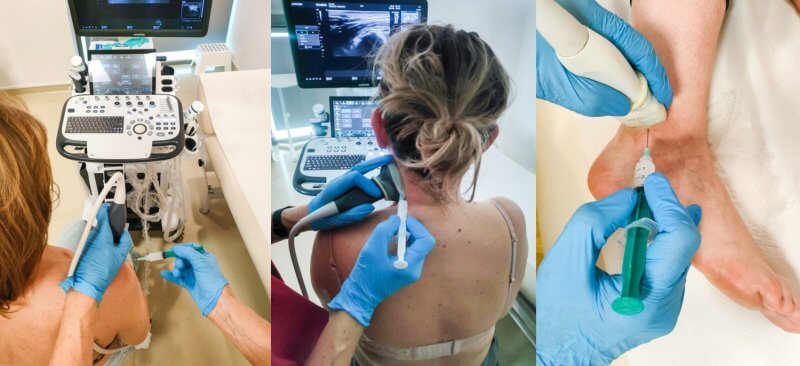
What Is the Course of an Ultrasound-Guided Procedure?
- Patient Preparation – The physician disinfects the skin at the treatment site and positions the patient to provide optimal access to the affected area.
- Ultrasound Visualization – The ultrasound probe is used to locate the target structure (e.g., calcification, cyst, joint), which is displayed in real-time on a monitor.
- Local Anesthesia – In most cases, a local anesthetic is administered to ensure a pain-free procedure.
- Instrument Introduction – Under continuous ultrasound guidance, the physician inserts a needle, cannula, or another fine instrument precisely into the target location, such as a joint, cyst, or tendon.
- The Procedure Itself – Depending on the indication, the procedure may involve fluid aspiration, drug administration, calcification flushing, tendon fiber release, or another precise intervention.
- Completion and Post-Procedure Care – After removing the needle, the puncture site is dressed, and the patient is given brief post-procedure instructions (e.g., limit movement for 24 hours).
The procedure is safe, minimally painful, and does not require hospitalization—patients typically return home immediately afterward.
How Long Does an Ultrasound-Guided Procedure Take?
The duration of a sonosurgical procedure depends on the type and complexity of the intervention, but generally falls within:
- 10–20 minutes for simple injections, aspirations, or nerve blocks
- 20–40 minutes for more complex procedures such as calcification removal, tenotomy, or cyst flushing
- Up to 60 minutes for multi-step procedures (e.g., combining flushing, injection, and mechanical tendon intervention)
A major advantage is that all procedures are performed on an outpatient basis—without the need for general anesthesia or hospitalization—and most patients can leave the clinic shortly afterward.

Are Sonosurgical Procedures Painful?
Sonosurgical interventions are generally minimally painful or even painless, primarily due to:
- Local anesthesia, which eliminates pain during the procedure
- Precise ultrasound control, which helps avoid unnecessary tissue trauma
- Use of very fine needles and instruments, which minimizes discomfort
Patients typically report only mild sensations of pressure, stretching, or a slight prick during needle insertion or drug delivery. After the procedure, slight tenderness or a "tight" feeling at the site of intervention may occur but usually resolves within 1–2 days.
Key Advantages of Ultrasound-Guided Procedures
- Precision – Real-time ultrasound allows exact localization of pathology and tool navigation with millimeter accuracy, minimizing the risk of damaging surrounding structures.
- Minimal Invasiveness – Procedures are performed through a small puncture, without skin incisions, stitches, or disruption of major tissues, significantly reducing trauma.
- No Hospitalization Required – These are outpatient procedures—patients can leave the clinic the same day, often returning to normal activities immediately.
- Lower Risk of Complications – Ultrasound control reduces the risk of bleeding, infection, and nerve or vessel injury. The absence of an open wound also lowers the risk of infection.
- Reduced Pain – The procedures are well-tolerated, performed under local anesthesia with fine instruments, and usually cause minimal or no post-procedural pain.
- Rapid Return to Function – Most patients resume normal activities within 24–48 hours, without needing extended leave or rehabilitation.
- Repeatability – Procedures can be repeated if needed, such as in cases of pain recurrence or during ongoing biologic therapies (e.g., PRP).