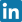Jednoczesny ból w pachwinie po prawej stronie i ból w pachwinie po lewej stronie.
Zagłębiając się jednak bardziej szczegółowo, okazuje się, że problem bywa często bardziej złożony – w środowisku medycznym niedawno użyto nawet stwierdzenia, że jest to „Trójkąt Bermudzki medycyny sportowej”.
Istotnymi czynnikami w różnicowaniu klinicznym bólu w pachwinie są odpowiedzi na pytania takie jak:
|
Jest to bardzo ważne, gdyż lokalizacja oraz jakość objawów jest pomocna podczas różnicowania klinicznego pomiędzy strukturami wewnątrz stawowymi i zewnątrz stawowymi oraz mięśniowo-szkieletowymi (mięśnie, więzadła, ścięgna, pochewki ścięgniste, powieź, obrąbek stawowy) i dolegliwościami spoza układu mięśniowo-szkieletowego (ból którego przyczyną jest układ moczowo-płciowy, a który prezentuje objawy w okolicy pachwiny).

Ból pachwiny - możliwe przyczyny
1. Ból w pachwinie w obrębie mięśni przywodzicieli, pacjenci czasem określają go jako naciągnięcie pachwiny
Ból ten jest jedną z najczęściej wymienianych dolegliwości w obrębie pachwiny. Główną funkcją tej grupy mięśniowej jest ruch przywiedzenia w biodrze oraz stabilizacja miednicy podczas fazy przeniesienia kończyny dolnej w chodzie. W odniesieniu do sportu, są one ważne w każdej dyscyplinie wymagającej nagłych zmian kierunku ruchu oraz gwałtownych ruchów kończyny dolnej, jak np. kopanie piłki. Bolesność palpacyjna (dotykowa) w obrębie przyczepów mięśniowych, kłucie w pachwinie, ból pachwiny przy chodzeniu lub ból biodra przy chodzeniu, ból przy rozciąganiu i napięciu izometrycznym (napięciu mięśnia wbrew oporowi bez wykonywania ruchu) są istotnymi klinicznie wskaźnikami. Najczęściej zapaleniu ulega przywodziciel długi, ze względu na jego najbardziej przednie położenie.
2. Ból pachwiny prowokowany przez mięsień biodrowo-lędźwiowy
Mięsień ten jest najsilniejszym zginaczem biodra, nazywany „mięśniem sprinterów”, pełniącym bardzo ważną rolę w utrzymywaniu odpowiedniej postawy ciała, chodzeniu oraz bieganiu. Najczęściej ulega on uszkodzeniu podczas aktywności wymagających powtarzanego zgięcia biodra, bądź rotacji zewnętrznej w stawie biodrowym takich jak: bieganie, gra w piłkę nożną, uprawianie gimnastyki. Ból w pachwinie po prawej stronie, jak i ból w pachwinie po lewej stronie występuje najczęściej podczas oporowego ruchu zgięcia w stawie biodrowym oraz rozciąganiu mięśni zginaczy biodra. Zapaleniu może ulec również kaletka znajdująca się pod przyczepem mięśnia przy krętarzu mniejszym (w obrębie pachwiny).
3. Uszkodzenie obrąbka stawowego a ból pachwiny
Obrąbek stawu biodrowego to gęsta, włóknista tkanka, która zapewnia dodatkową stabilność w stawie. Obrąbek może ulec pęknięciu lub zwyrodnieniu. Objawem uszkodzenia może być trzaskanie podczas ruchu w biodrze (biodro trzaskające) z bólem umiejscowionym głęboko w pachwinie.
4. Ból pachwiny a konflikt udowo-panewkowy
W tym wypadku ból zazwyczaj pojawia się podczas ruchu zgięcia biodra, rotacji wewnętrznej i przywiedzenia. Często odczuwalny jest ból w pachwinie przy chodzeniu. Zmiany w strukturze budowy kostnej głowy kości udowej bądź panewki stawu biodrowego mogą prowokować dolegliwości bólowe na skutek nieprawidłowego działania sił kompresyjnych na tkanki. Dolegliwości mogą przypominać uczucie „ściskania” w biodrze nasilającego się podczas zwiększania zakresu ruchu zgięcia np. podczas przyciągania kolana do brzucha po skosie, czy przy wykonaniu skłonu w przód w siadzie z nogą na nodze, gdy bolesna kończyna znajduje się na górze. Ból może wywoływać również mniej złożony ruch, jak chociażby jedynie skłon w przód w staniu, czy w siadzie. Przeczytaj jak złagodzić ból pachwiny powodowany przez konflikt udowo-panewkowy.
5. Zapalenie w obrębie spojenia łonowego a ból w pachwinie
Zapalenie to objawia się bólem zlokalizowanym centralnie nad spojeniem łonowym, może promieniować do dolnych partii brzucha, może to być ból w pachwinie promieniujący na nogę, na wewnętrzną stronę uda bądź narządów płciowych. Bierne rozciąganie mięśni przywodzicieli oraz aktywne napięcie wbrew oporowi prowokuje objawy – podobnie jak w różnicowaniu bólu prowokowanego przez stan zapalny przyczepu mięśni przywodzicieli. Podobieństwo objawów wynika z tego, że anatomicznie przyczep przywodziciela długiego (jednego z całej grupy mięśni wewnętrznej strony uda) oddaje również swoje włókna do więzadeł w obrębie spojenia łonowego. Często towarzyszące są zmiany dysfunkcyjne stawu krzyżowo-biodrowego. W badaniu RTG widoczne są nieregularne brzegi kości łonowej przy spojeniu łonowym, poszerzona szpara stawowa. Lekarz może zlecić badanie RTG w staniu na jednej nodze, co prowokuje działanie sił ścinających na staw i może wygenerować widoczne asymetrie występujące przy braku stabilności więzadłowej.
6. Złamania zmęczeniowe
Złamaniu zmęczeniowemu może ulec szyjka kości udowej. Pomimo zazwyczaj rzadko występujących komplikacji w przypadku wczesnej interwencji, w momencie lekceważenia długotrwałych objawów bólowych, może dojść do pełnego złamania, również z przemieszczeniem. Ból w pachwinie przy chodzeniu zazwyczaj narasta wraz z pokonywanym dystansem, w bardziej zaawansowanych przypadkach pojawia się również w nocy. Lokalna palpacja (badanie dotykiem) raczej nie odtwarza objawów pacjenta, jednak obronne napięcie mięśniowe spowodowane bólem może uczynić badanie nieprzyjemnym.
7. Przepuklina pachwinowa
Dysfunkcja ta dotyczy zmian w tylnej ścianie jamy brzusznej, nie jest wyczuwalna dotykiem, gdyż dotyczy tkanek położonych głęboko w powięzi. Ból w pachwinie lewej, tak samo jak ból w pachwinie prawej może promieniować do mięśni przywodzicieli, krocza, moszny. Ważną informacją jest to, że ból nie występuje w spoczynku, ale jest związany z ruchem, np. kopanie, zmiany kierunku ruchu. Jest trudna w diagnostyce, oceniana podczas badania USG z jednoczesnym zwiększeniem ciśnienia w jamie brzusznej przez pacjenta przez próbę oporowego wydechu na wdechu. Lekarz ocenia ciągłość tkanek oraz możliwe „wybrzuszenia tkanek” przez tylną ścianę jamy brzusznej do kanału pachwinowego.

8. Ból pachwiny a dolegliwości kręgosłupa lędźwiowego
Przepuklina dysku międzykręgowego może prowokować dolegliwości około pachwinowe. Dotyczy to głównie przepuklin znajdujących się na wyższych segmentach kręgosłupa lędźwiowego (L1-L3), jednakże przepuklina kręgosłupa z segmentów położonych niżej (L4-L5, L5-S1) również może powodować takie dolegliwości w obrębie pachwiny co potwierdzają liczne badania.
9. Uwięźnięcie nerwu a ból w pachwinie
Jako kolejna z możliwych przyczyn, powoduje wrażenie pieczenia oraz zaburzeń czucia w okolicach zaopatrywanych przez konkretną gałązkę nerwu (np. n. płciowo-udowy, n. biodrowo-podbrzuszny, n. biodrowo-pachwinowy, n. zasłonowy, n. skórny boczny uda, n. sromowy, n. udowy). Zaburzone czucie może występować w okolicy podbrzusznej poniżej lub powyżej gdzie przebiega więzadło pachwinowe, wewnętrznej strony uda, przedniej zewnętrznej strony uda, narządów płciowych. Warto również zwrócić uwagę na osłabienie siły mięśniowej, gdyż to również może być wskaźnikiem ucisku/uwięźnięcia gałązki nerwu (np. n. udowy, n. zasłonowy). Istotną informacją kliniczną są przebyte wcześniej zabiegi operacyjne, ponieważ nerw może ulec uwięźnięciu nawet w tkance bliznowatej i sprowokować dolegliwości od tygodnia po zabiegu, aż do miesięcy czy nawet lat.
10. Dolegliwości spoza układu mięśniowo-szkieletowego
Ból z boku tułowia, promieniujący do pachwiny, oraz występujący krwiomocz może wskazywać na choroby nerek. Zapalenia najądrza, jąder u mężczyzn, czy problemy ginekologiczne u kobiet – endometrioza, cysty na jajnikach, mogą promieniować do pachwiny. Szereg dolegliwości takich jak: kamica nerkowa, skręcenie przydatków, zapalenie wyrostka robaczkowego, zapalenie jądra, tętniak aorty brzusznej również należy wykluczyć podczas przeprowadzania diagnostyki. Ból podczas stosunku płciowego też jest informacją istotną klinicznie, o której warto pamiętać podczas rozmowy z lekarzem jak złagodzić ból pachwiny.
11. Ból pachwiny, szczególnie u osób starszych, może być wywołany zmianami zwyrodnieniowymi stawu biodrowego.
Boli Cię pachwina? Znajdź ortopedę z Rehasport w popularnych lokalizacjach: |
Ból w pachwinie - diagnostyka różnicowa
W celu postawienia trafnej diagnozy, jak złagodzić ból pachwiny, przeprowadza się szereg testów klinicznych (badanie manualne), które potwierdzane są zleconymi przez lekarza badaniami dodatkowymi. Pacjent jest przede wszystkim oceniany wizualnie poprzez oglądanie bolesnej okolicy pachwiny oraz przylegających struktur w celu oceny sylwetki, asymetrii oraz atrofii mięśniowej (zmniejszenie masy brzuśca mięśniowego). Ocenie podlega: biodro (zakresy ruchu, badanie siły mięśniowej, palpacja oraz testy specyficzne), staw krzyżowo-biodrowy, spojenie łonowe, jama brzuszna oraz odcinki kręgosłupa - kręgosłup lędźwiowy. Przeprowadzana jest w różnych pozycjach: w staniu, leżeniu, obserwacji podlegają również chód oraz czynności funkcjonalne. Istotne klinicznie są także: różnice w wysokości talerzy biodrowych, długość kończyn czy rotacja talerza biodrowego. Każdy ból w lewej pachwinie, jak i ból w prawej pachwinie odczuwany przez pacjenta jest notowany i podlega ocenie. W zależności od rodzaju objawów, jak złagodzić ból pachwiny, lekarz może zlecić badania takie jak: MRI (rezonans magnetyczny), USG (również dynamiczne USG), RTG.
Tabletki na ból pachwiny
Leczenie bólu pachwiny często jest wieloetapowe. Oprócz fizjoterapii ortopeda może zalecić leczenie farmakologiczne. Jest ono zależne od przyczyny dolegliwości bólowych. W przypadku bólu spowodowanego stanem zapalnym lekami pierwszego wyboru są niesteroidowe leki przeciwzapalne (NLPZ) zarówno w formie doustnej, jak i miejscowej (maści, żele itp). Jeżeli ból związany jest z uszkodzeniem chrząstki stawowej zastosowanie znajdują preparaty chon.droprotekacyjne. Ból pachwiny będący związany z problemami na poziomie kręgosłupa lędźwiowego można leczyć lekami zmniejszającymi napięcie mięśniowe oraz lekami zawierającymi witaminy z grupy B. W przypadku chorób pozaortopedycznych (takich jak problemy ginekologiczne, urologiczne lub chirurgiczne) leczenie może wymagać innych leków, które zaordynuje lekarz stosownej specjalności.
Ćwiczenia na ból pachwiny - rehabilitacja (leczenie zachowawcze)
Rehabilitacja powinna być zindywidualizowana. Biorąc pod uwagę szereg czynników biomechanicznych, każdy przypadek, pomimo podobnych objawów, może charakteryzować się odmienną przyczyną, co powinno zostać szczegółowo przeanalizowane przez prowadzącego fizjoterapeutę. Przyczynami biomechanicznymi może być zarówno dysbalans mięśniowy w obrębie stawu biodrowego, jak i kręgosłupa lędźwiowego, czy całej obręczy miedniczej. Przy braku stabilizacji ze strony mięśni tułowia koncentrowanie działań jedynie na stawie biodrowym może nie przynieść pożądanego efektu. Przyczyną wprowadzenia treningu stabilizacyjnego jest fakt transferu (przeniesienia działania) sił mięśni przez tułów na biodro, co przy nieodpowiednim rozkładzie działania sił może prowadzić do dysfunkcji. Nadmierne napięcia mięśniowe, brak elastyczności, brak zakresu ruchu, brak stabilizacji to kluczowe elementy podlegające ocenie fizjoterapeutycznej.
Fizjoterapeuta ocenia relacje w sile mięśniowej aparatu stabilizującego staw biodrowy: mięśnie zginacze, prostowniki, przywodziciele, odwodziciele oraz rotatory. Istotnym elementem jest elastyczność mięśniowa, umożliwiająca wykonanie pełnego zakresu ruchu w stawie biodrowym. Przy występujących zmianach wewnątrz stawu z obkurczeniem torebki stawowej, działania ukierunkowane jedynie na stretching i wzmacnianie mięśni powinny iść w parze z mobilizacją manualną. Często występujący u osób z dolegliwościami bólowymi pachwiny deficyt rotacji wewnętrznej w stawie biodrowym powoduje nawracające stany zapalne w obrębie przyczepów mięśni przywodzicieli.
Ćwiczenia na ból pachwiny muszą zostać wyjaśnione pacjentowi i ew. skorygowane, gdyż często brak dokładności w wykonywaniu ćwiczeń rehabilitacyjnych przekłada się na brak efektu terapii. W miarę upływu czasu zestaw ćwiczeń ulega zmianie wraz ze zmieniającym się stanem czynnościowym pacjenta. Ćwiczenia powinny również spełniać wymagania pacjenta co do wyznaczonego celu końcowego. U sportowców bardzo istotna jest adaptacja tkanek do stopniowo zwiększających się obciążeń oraz płynne przejście w specyficzny dla danej dyscypliny sportowej trening motoryczny.
W Rehasport rehabilitację dostosowujemy do każdego pacjenta indywidualnie. Znajdź fizjoterapeutę w popularnych lokalizacjach: |
Prezentowane przez fizjoterapeutkę mgr Adriannę Wojewódzką przykładowe ćwiczenia na ból pachwiny są jedynie propozycją, każdy pacjent powinien otrzymać indywidualnie dostosowany przez rehabilitanta program ćwiczeń adekwatny do występujących deficytów ruchowych. Każdy pacjent powinien być również odpowiednio skorygowany przez fizjoterapeutę w celu poprawnego wykonania ćwiczeń unikając kompensacji w wykonywanych ruchach.
Ból w pachwinie - ćwiczenie 1
Pozycja wyjściowa – leżenie na boku, tyłem do ściany. Pacjent wykonuje ruch odwiedzenia w stawie biodrowym przesuwając piętę po ścianie w górę i w dół, utrzymując miednicę stabilną, w pozycji neutralnej.
Należy zwracać uwagę, aby unikać błędnego wzorca ruchowego, ustawiając miednicę w przodopochyleniu (plecy „przeprostowują się” ) i podnoszeniu zbyt wysoko kończyny dolnej.
Ból w pachwinie - ćwiczenie 2
Pacjent, stojąc na jednej nodze, utrzymuje stabilną pozycję na dysku sensomotorycznym bądź innej formie niestabilnego podłoża.
Należy zwracać uwagą na prawidłowość wykonania ćwiczenia, aby nie robić nadmiernych ruchów ciałem, aby kończyna dolna była w osi, a kolano nie uciekało do wewnątrz.
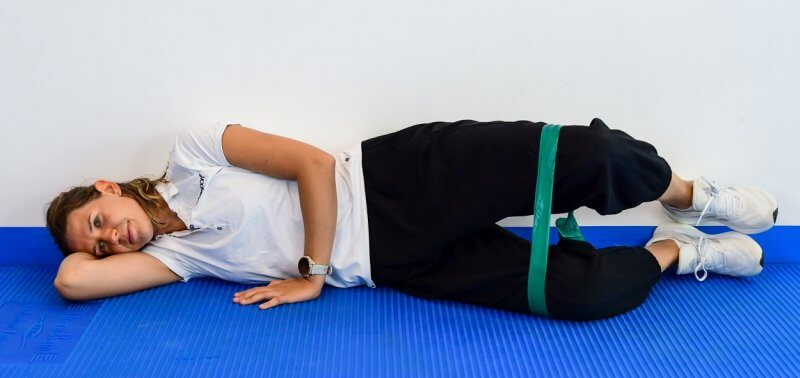
Ból w pachwinie - ćwiczenie 3
Leżenie bokiem, nogi ugięte w kolanach, nad kolanami znajduje się guma elastyczna o stopniu oporu dobranym indywidualnie. Pacjent wykonuje ruch odwiedzenia w stawie biodrowym unosząc kolano i utrzymując złączone pięty wbrew oporowi gumy.
Ból w pachwinie - ćwiczenie 4
W staniu w półprzysiadzie z gumą elastyczną zaczepioną nad kolanami. Pacjent utrzymując stopy stabilnie na podłożu wykonuje ruch odwiedzenia w stawach biodrowych w możliwym dostępnym zakresie ruchu bez zmiany pozycji stóp, a następnie wraca do pozycji wyjściowej.
Ból w pachwinie - ćwiczenie 5
Pacjent zaczyna ćwiczenie z pozycji 1/4 przysiadu bokiem do drabinki z gumą zaczepioną ponad stawem skokowym. Wbrew oporowi gumy pacjent powoli odstawia kończynę do boku – ruch odwiedzenia w stawie biodrowym, a następnie powraca do pozycji wyjściowej łącząc nogi. W tym ćwiczeniu stawiamy nacisk na pracę mięśni przywodzicieli oraz utrzymanie prawidłowej pozycji kończyny stabilnej.
Ból w pachwinie - ćwiczenie 6
Pacjent znajduje się w pozycji leżącej na plecach bokiem do drabinki, kolana ugięte. Taśma elastyczna zaczepiona jest nad stawem kolanowym. Pacjent powoli wbrew oporowi gumy hamuje ruch zbliżania się kolana do drabinek, a następnie zbliża kolana wracając do pozycji wyjściowej.
Ćwiczenia zamieszczone powyżej są jedynie propozycją, jednak aby osiągnąć skuteczność, należy ich wykonanie i stosowność w konkretnym przypadku skonsultować z fizjoterapeutą.
Powiązane artykuły:
Poznaj inne możliwe przyczyny powodujące ból biodra.
Bibliografia
- Hackney RG., (iv) Groin Pain in Athletes. Orthopaedics and Trauma 2012; 26 (1): 25 – 32.
- Robinson P, Chopra A., Imaging Athletic Groin Pain. Radiologic Clinics of North America 2016; 54: 865 – 873.
- Weir A, Jansen JACG, van de Port IGL, et al., Manual or exercise therapy for long – standing adductor – related groin pain: A randomized controlled clinical trial. Manual Therapy 2011; 16: 148 – 154.
- Jones NS., Update: Soccer Injury and Prevention, Concussion and Chronic Groin Pain. Current Sports Medicine Reports 2014; 13 (5): 319 – 325.
- Rafin BS, Tang L, Nielsen MP, et al., Hip Strenght Testing of Soccer Players With Long – Standing Hip and Groin Pain: What are the Clinical Implications of Pain During Testing? Clinical Journal of Sports Medicine 2016; 26: 210 – 215.